According to the 2020 Global Cancer Burden data released by the International Agency for Research on Cancer (IARC), breast cancer accounted for a staggering 2.26 million new cases worldwide, surpassing lung cancer with its 2.2 million cases. With an 11.7% share of new cancer cases, breast cancer ranks first, making it the most common form of cancer. These numbers have raised awareness and concern among countless women regarding breast nodules and breast masses.
What You Need to Know About Breast Nodules
Breast nodules typically refer to lumps or masses found in the breast. Most of these nodules are benign (non-cancerous). Some common benign causes include breast infections, fibroadenomas, simple cysts, fat necrosis, fibrocystic changes, and intraductal papillomas.
Warning Signs:
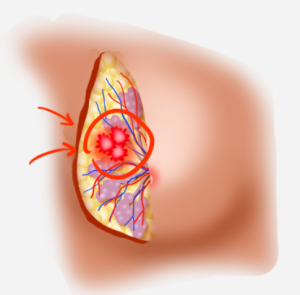
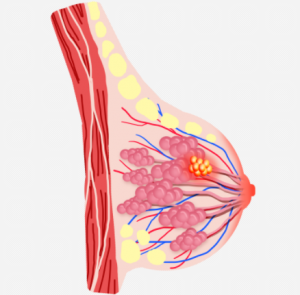
However, a small percentage of breast nodules can be malignant (cancerous), and they may exhibit the following warning signs:
- Size: Larger nodules tend to raise concerns more easily.
- Shape: Nodules with irregular or jagged edges have a higher likelihood of malignancy.
- Texture: If a nodule feels hard or has an uneven texture upon touch, further investigation is needed. This is especially important for women over 50 years old, as the risk of malignancy increases with age.
Breast Nodule Examination and the Significance of Early Diagnosis of Breast Cancer
Studies have shown that while the incidence of breast cancer is increasing, the mortality rate from breast cancer has been declining in Western countries over the past decade. The primary reason for this decline can be attributed to the optimization of early diagnosis and treatment methods, with breast cancer screening being a key component.
1. Examination Methods
- Currently, research on the sensitivity differences between different examination methods mainly comes from Western countries. Clinical breast examinations have lower sensitivity compared to imaging techniques. Among imaging methods, magnetic resonance imaging (MRI) has the highest sensitivity, while mammography and breast ultrasound have similar sensitivities.
- Mammography has a unique advantage in detecting calcifications associated with breast cancer.
- For lesions in dense breast tissue, breast ultrasound has significantly higher sensitivity than mammography.
- Adding whole-breast ultrasound imaging to mammography can significantly increase the detection rate of breast cancer.
- Breast cancer is relatively more common in premenopausal women with high breast density. Therefore, the combined use of mammography and whole-breast ultrasound imaging is more reasonable.
- For the specific symptom of nipple discharge, intraductal endoscopy can provide a direct visual examination of the breast duct system to detect any abnormalities within the ducts.
- Breast magnetic resonance imaging (MRI) is currently recommended internationally for individuals at high risk of developing breast cancer throughout their lifetime, such as those carrying pathogenic mutations in BRCA1/2 genes.
2.Regular Breast Self-Examination
Breast self-examination has been encouraged in the past, but recent research indicates that it does not reduce breast cancer mortality. The 2005 edition of the American Cancer Society (ACS) guidelines no longer recommends monthly breast self-examinations as a method for early detection of breast cancer. However, regular breast self-examination still holds some value in terms of potentially identifying breast cancer at later stages and detecting cancers that may occur between routine screenings.
3.Significance of Early Diagnosis
Early diagnosis of breast cancer has several significant benefits. For example, detecting non-invasive breast cancer can potentially avoid the need for chemotherapy. Additionally, early detection of breast cancer provides more opportunities for breast-conserving treatment, which preserves the breast tissue. It also increases the chances of avoiding axillary lymph node dissection surgery, which can cause functional impairments in the upper limbs. Therefore, timely diagnosis allows for more options in treatment and reduces the potential impact on quality of life.
Methods and Criteria for Early Diagnosis
1. Early Diagnosis: Early Breast Lesions and Pathological Confirmation
Recent research results show that breast cancer screening using mammography can reduce the annual risk of breast cancer death by 20% to 40%.
2. Pathological Examination
- Pathological diagnosis is considered the gold standard.
- Each imaging method has corresponding pathological sampling methods. Since most asymptomatic lesions discovered are benign, the ideal method should be accurate, reliable, and minimally invasive.
- Ultrasound-guided core needle biopsy is currently the preferred method, applicable to over 80% of cases.
3. Key Aspects of Early Diagnosis of Breast Cancer
- Positive mindset: It is important not to ignore breast health but also not to fear. Breast cancer is a chronic tumor disease that is highly responsive to treatment. With effective treatment, most cases can achieve long-term survival. The key is active participation in early diagnosis to minimize the impact of breast cancer on health.
- Reliable examination methods: In professional institutions, a comprehensive approach combining ultrasound imaging and mammography is recommended.
- Regular screening: Starting from the age of 35 to 40, it is recommended to have a breast examination every 1 to 2 years.
Post time: Aug-11-2023



